23 December 2020
Rheumatic Pain
Rheumatic pain is simply pain caused by something under the umbrella of rheumatology. Rheumatology is a hard speciality to define, but it definitely includes:
- Rheumatoid Arthritis
- Ankylosing Spondylitis and AxSpA
- Polymyalgia Rheumatica (PMR)
- Psoriatic Arthritis
These are autoimmune conditions that affect the joints, so they may lead someone to seek osteopathic treatment. This means that the body attacks its own cells and that is what causes the pain and other symptoms. Although we can't cure rheumatoid conditions, we can help with the symptoms.

Rheumatoid Arthritis (RA)
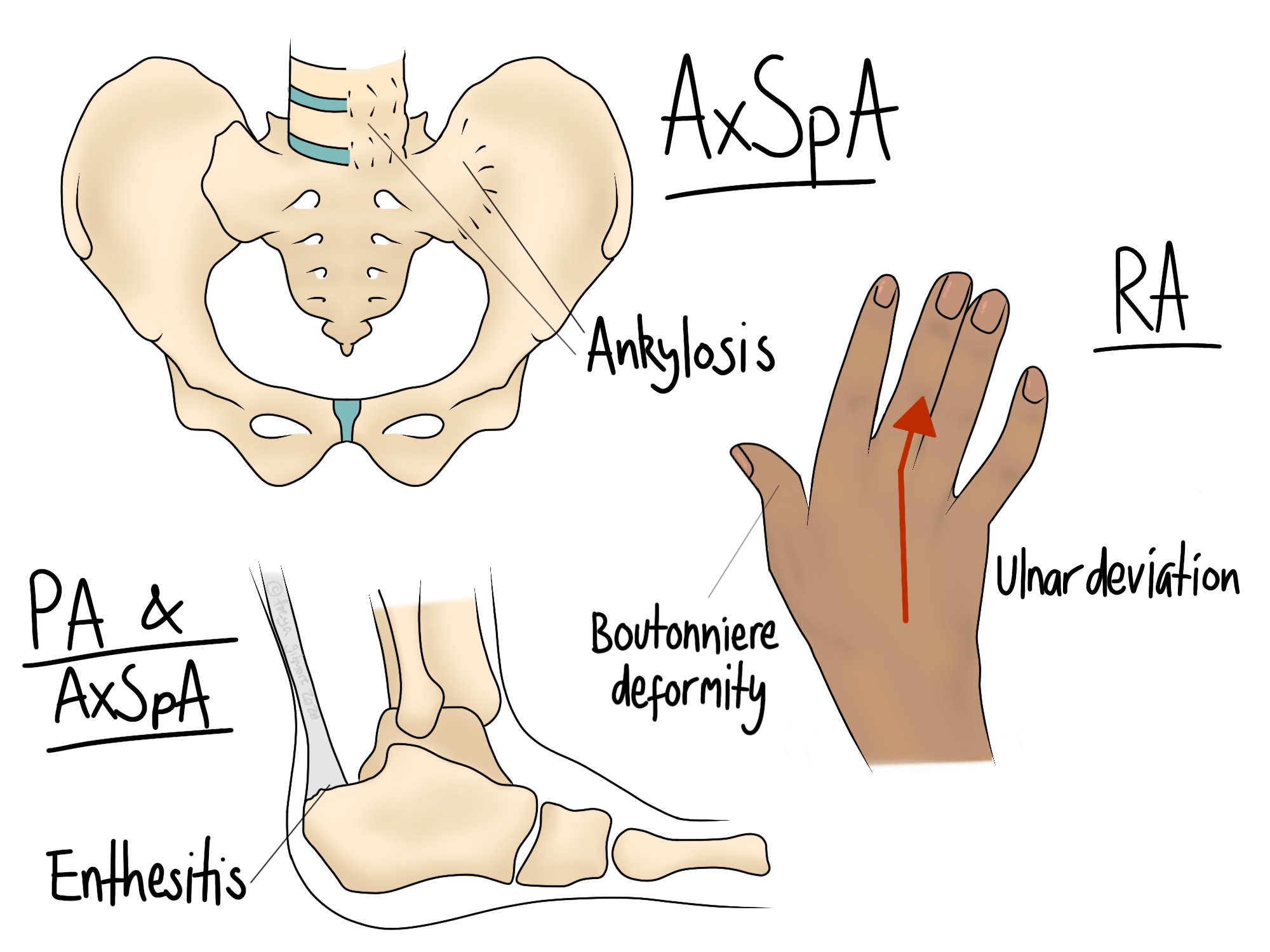
RA is an autoimmune condition affecting the joints. It is most commonly seen in the small joints such as the hands and neck. Symptoms may also affect the hips and knees. Inflammation within the joints leads to destruction of the cartilage and underlying bone. This leads to pain and stiffness, and in some joints there is some deformity. The wrists may turn outward (ulnar deviation) and the fingers may develop lumps on the joints, or a "swan neck" deformity.
RA symptoms follow a number of patterns. Some people have them consistently, others relapse and remit, and a few only have a single episode. Alongside joint symptoms, patients might develop lung or skin problems. There are also links to crohn's disease and ulcerative colitis.
Full post coming in April
Ankylosing Spondylitis (AS) and AxSpA
AxSpA is short for Axial Spondyloarthropathy: this literally means "joint condition of the spine". It covers the early stages of AS. The two are inflammatory conditions in which the body attacks the joints of the spine and pelvis. When inflammation subsides, the body heals incorrectly, laying down bone over the joints. This leads to episodes of pain followed by increasing fusion and stiffness.
AS is heavily underdiagnosed. Early symptoms can make it look like persistent lower back pain, which may never be fully investigated. There's also some misunderstanding professionally, that you can't have AS unless you have the "question mark posture".
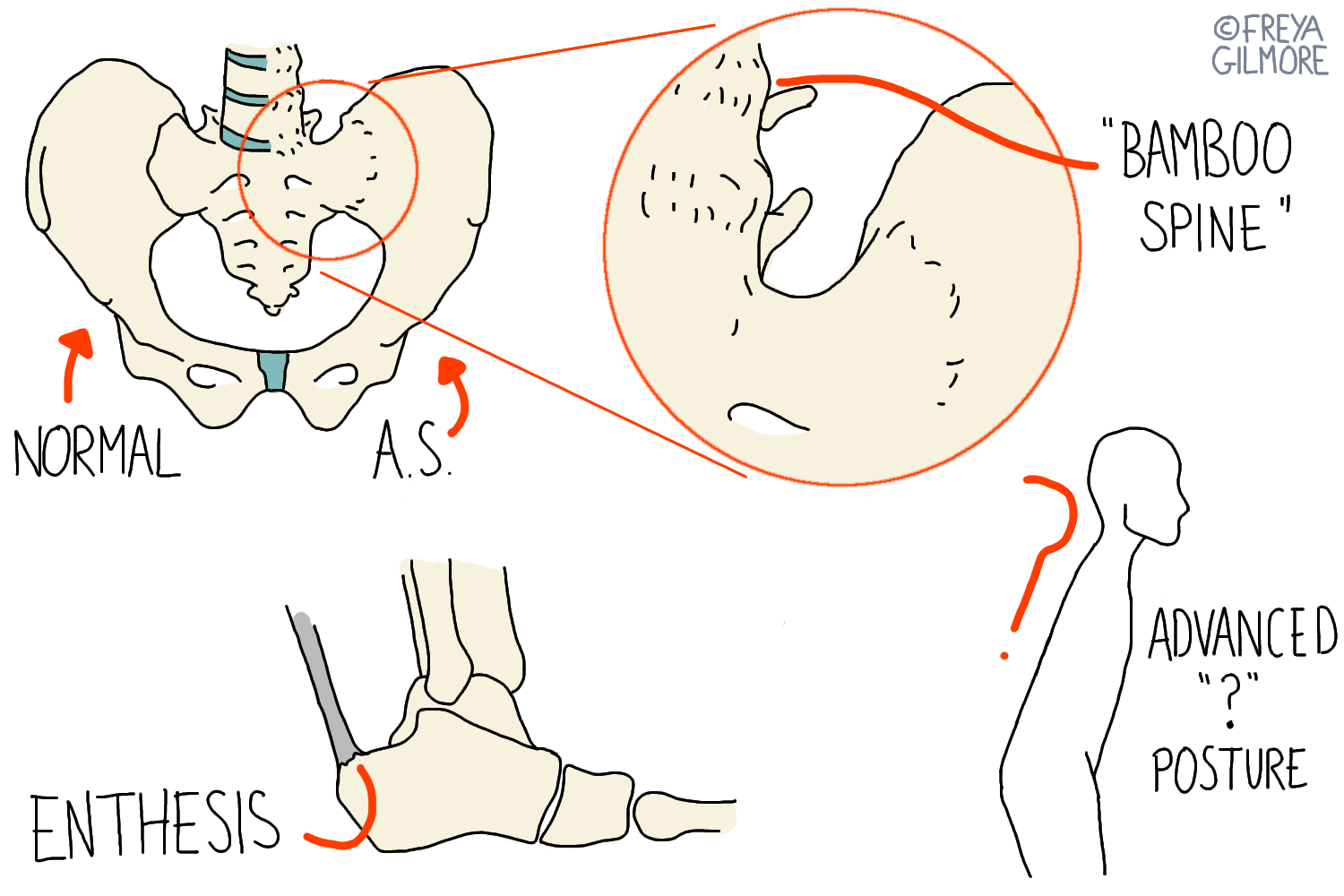
However, the posture in question is a sign that the disease has advanced a long way. Catching the condition early is important for management and treatment. Strong drugs are available to help slow the progress of AxSpA, but they need to be prescribed by a rheumatologist.
Stay tuned for a full post on AS and AxSpA coming in April.
Psoriatic Arthritis
Another rheumatic condition with a more familiar name is psoriatic arthritis. This affects about 10% of people who have psoriasis. Its symptoms have a lot of overlap with the conditions above. Enthesitis (inflammation where a tendon meets bone) and lower back or pelvis pain feature here, as they do with AxSpA.
Joints under skin affected by psoriasis may be particularly prone to this arthritis. Hands, feet, hips, and knees are commonly affected.
Some of the hallmarks that the other rheumatic conditions above don't cause affect the hands. Fingers may swell and take on a red tone, and the nails may change texture.
Managing Rheumatic Pain
Inflammation is worst at rest, so exercise and hands on therapy can help with symptoms. By extension, some conditions may progress slower with management of inflammation.
However, these conditions can also be aggravated by doing too much at once as well. Your osteopath will take this into account when devising your treatment plan. This might mean that some days it is only appropriate to do a short or light treatment, but if you have other aches and pains, they might be safe to treat.
As mentioned above, your osteopath can help you advocate for yourself when you need more medical support. We have the luxury of time as well as experience with musculoskeletal conditions. We see a lot of back pain, so we are well placed to tell when something isn't quite right. Rheumatic conditions typically require formal diagnosis by a rheumatologist, which will likely need a referral from your GP. Your osteopath can write a letter to explain their findings and ask for further investigation.
If you're looking for support for rheumatic pain, book an appointment today.
Learn more
At Ilminster Osteopathy my goal is to help people achieve their goals whatever they may be. Watch our video to find out more.

